Insulin
The metabolism in the body requires the hormone insulin. It transports the glucose from the blood into the cells where it is needed for energy production. The carbohydrates from food are broken down in the intestines, among other things into glucose. These glucose molecules enter the blood and are distributed from there to the cells of all parts of the body. The insulin opens the cells for the sugar molecules.
If you are a person with diabetes who needs insulin injections, this means that your body cannot produce enough of its own insulin. If there is a lack of insulin blood glucose levels will increase rapidly and can result in a ketoacidosis or even in a ketoacidotic coma. However, thanks to individually tailored insulin therapy, you can lead a largely unrestricted, active and healthy life.
Self-responsible specialist
Insulin-dependent people with diabetes have to know exactly about action of the used insulins. But more than that. They need to understand how insulin, diet and activity work together to ensure that the required insulin level is always present in the blood. Intensive education is necessary to enable the self-responsible specialist to manage his life nearly like a healthy individual. This is important for both people with type 1 and type 2 diabetes. Different actions of insulin enable people to reach a high flexibility including high level of training activity.
Adaption of insulin delivery to daily life situations
Whenever food intake or training activities differ a lot from standard daily life situations the insulin dose has to be adequately adapted. You can control your measures by testing blood glucose more often. If your blood glucose levels keep to be elevated for a longer period of time it is necessary to adapt the insulin dose following the concepts of your physician.
The production of Insulin
Insulin was first discovered in the pancreas and explored by two Canadian scientists named Dr. Rederick G. Banting and Charles H. Best.in the year 1921. Until the Eigthies of the last century insulin was produced using pancreata from pigs and cattle. Today almost all people with diabetes use biosynthetic produced regular insulin which is processed from recombinant genetic technology. Microorganisms like medicinal yeast are programmed to produce insulin which is identical with human insulin.
Types of Insulin
There are 2 main types of insulin: regular insulin and insulin analogues. Within both groups we distinguish between short-, middle-, long-acting and mixes insulins. They differenciate from each in terms of taking effect, when strongest effect is reached and how long the effect takes place. The reason for that is that they are slightly different in structure and therefore the resorption form fatty tissue into blood takes different time. The choice of insulin for a person with diabetes depends on lifestyle and needs. The decision for the insulin of choice is taken together from the physician and the well-educated person concerned.
More information:
Types of insulin therapy
Injection technique
Concentration of Insulin
In most of the countries only U100 insulin is available (1 ml of liquid contains 100 I.U. of insulin). Please be aware when travelling in other countries that insulin with different concentration might be available (U40).
Take care to use the correct insulin concentration to avoid under- or overdosing!
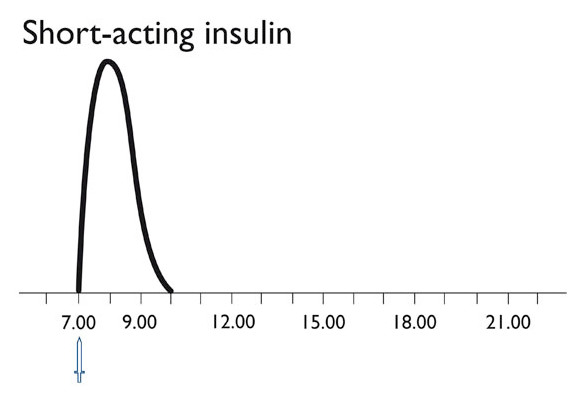
Short acting insulin
Analogue insulin
The effect of short acting insulin will start immediately after injection (10 minutes after injection). The peak of the effect is developed after 60 (30 to 90) minutes. In total the action will continue for two to three hours. Please refer to the graph below to get more information about the spectrum of the effect.
Due to this rapid onset on action of these new short time insulins (analogue insulins) it is not necessary to wait between injection of insulin and the meal if the blood glucose result is OK. Analogue insulins can be injected before, during or immediately after the meal which provides a high grade of flexibility.
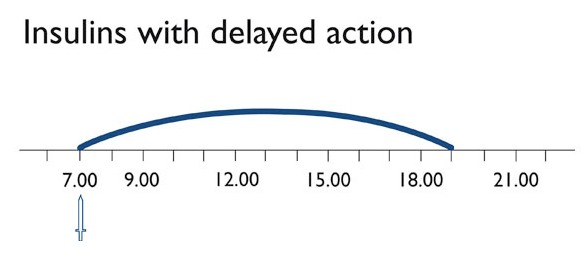
Delayed insulin
Delayed insulin covers the body's constant basic need for insulin and is therefore also called basal insulin (fasting insulin).
There are the following main groups of long-acting insulins:
- NPH-insulin (can be injected by means of an insulin pen)
- Zinc-insulin (cannot be injected by means of an insulin pen)
- analogue insulins with delayed action: glargine, detemir, glulisin (can be injected by means of an insulin pen)
NPH-insulin
NPH stands for Neutral Protamin Hagedorn. It is released slowly and provides an effect of middle term duration. Insulin is bound to the carrier NPH which causes the delay of resorption into the blood. Due to the dose the delay can be different. Normally the duration of the effect is 12 (8 – 16) hours. The peak of the effect develops after 4 to 6 hours.
Zinc insulins
Depending on the grade of crystallization of insulin they provide middle term (12 – 16) to long term (24 – 46) duration of the effect.
Analogue insulins with delayed action
One of the newer developments of insulin analogues are analogues with delayed action like glargine, detemir or glulisin. Their duration of effect ist longer (average 24 hours) than from NPH insulin, they act more constantly and decrease therefore the risk of a hypoglycaemia.
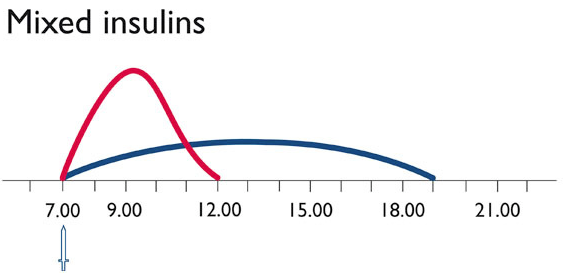
Mixed Insulin
Regular and NPH insulins with delayed action can be mixed. The resulting NPH mixes insulins can be adapted to the individual needs of a person with diabetes. The pharmacodynamics of both components will stay the same.
NPH-mixed insulins are available in different defined relations also in ready injection pens.
Mixed analogues are ready mixtures from short-acting insulin analogues and a component with delayed action.
The short-acting part covers the insulin need for meals whereas the component with delayed action takes care for basal needs. Mixes analogues can be injected direct at the meal and the risk to develop a hypoglycaemia is reduced. Blood glucose levels after the meal are better in comparison to injections of mixed insulins containing regular insulin.
More information:
Oral Antidiabetics
Types of insulin therapy
Injection technique